 Rwanda is fighting its first outbreak of the Marburg virus and experiencing its third-largest outbreak. As of October 2024, there were 63 cases, with 15 cases resulting in death. The Marburg virus is very contagious but only contracted through bodily fluids and scientists believe the Rwanda outbreak began with contact with contaminated animals.
Rwanda is fighting its first outbreak of the Marburg virus and experiencing its third-largest outbreak. As of October 2024, there were 63 cases, with 15 cases resulting in death. The Marburg virus is very contagious but only contracted through bodily fluids and scientists believe the Rwanda outbreak began with contact with contaminated animals.
Animal Contagion
The Marburg outbreak in Rwanda was announced on September 27, 2024, according to Nature. Surrounding countries reported their outbreaks years before, with Tanzania and Equatorial Guinea having their outbreak just last year. At first, the virus’s origins were uncertain; researchers thought it came from an animal but had no proof. Rwanda started contract tracing and an epidemiological investigation to identify the first patients and to determine how they contracted the virus.
According to the World Health Organization (WHO), the animal of contact was possibly a Rousettus bat, a fruit bat found in mines or caves, because they carry the Marburg virus. “Initially, human Marburg virus infection results from prolonged exposure to mines or caves inhabited by Rousettus bat colonies,” said eMedicine Health.
Progress of the Marburg vaccine
The Marburg virus is a relative of the Ebola virus, both being part of the Filoviridae family. Both viruses have similar symptoms and transmission. According to eMedicineHealth, the Ebola virus has a higher fatality rate of 25%-90% compared to the Marburg virus fatality rate of 24%-88%. Ebola is more virulent but has two licensed vaccines, while the Marburg virus has none.
As of October 2024, the only vaccine for the Marburg virus is experimental. The scientists had the first trial of the experimental vaccine to fight the Marburg virus outbreak in early October. The Sabin Vaccine Institute sent out 700 vaccine doses to health care workers because they are the most at risk. The vaccine is currently in Phase 2, which means it is still undergoing testing. The Sabin Vaccine Institute still monitors people with previous outbreaks in surrounding countries.
“Interim results are expected next year, and Sabin also plans to launch a similar Phase 2 trial in the U.S. next year,” said the Sabin Vaccine Institute.
Outside Help
The people of Rwanda are not combating the Marburg virus outbreak alone. They have the support of many, some of which are WHO, Africa CDC and the United States, using a “governmental approach.” The CDC and WHO worked with Rwanda to begin a response to the outbreak and identify the public health needs. Rwanda’s supporters also sent scientists and researchers to help with the epidemiologic investigation and distribution of the vaccine.
The Marburg virus outbreak in Rwanda has reached level two for travelling which states “Practice Enhanced Precautions.” The WHO and the CDC have released statements about the outbreak and the risks people take if they travel to Rwanda. The supporters of Rwanda during the outbreak have helped create a response plan/program to assist in the public health of the people in Rwanda.
Conclusion
Since the announcement of the Marburg virus outbreak in Rwanda, the country has worked effortlessly to stop the virus. Many have come to Rwanda’s aid in their time of need. Their supporters have provided vaccines and plans to help support the public and the health officials/workers. Coming to Rwanda’s aid has allowed the progress of attaining an official and approved vaccine for the Marburg Virus that could prevent any more severe outbreaks in the future.
– Ashley Diaz
Ashley is based in Homestead, FL, USA and focuses on Global Health for The Borgen Project.
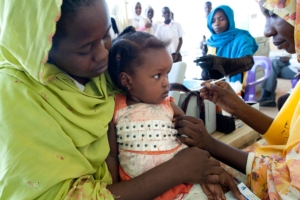
Photo: Flickr








 For many people around the world, the COVID-19 pandemic was an eye-opening event that revealed the dangers and inadequacies of the world’s global health systems. However, for other people, outbreaks of epidemic diseases might be more of a lived reality. On the continent of Africa, many know a certain geographic region in sub-Saharan Africa as the “meningitis belt.” These 26 countries face the dangers of meningitis more than other places around the world, and the outbreak of the COVID-19 pandemic delayed the vaccination of the MenAfriVac meningitis vaccine to 50 million children in these countries. African governments collaborated with the World Health Organization (WHO), the Bill and Melinda Gates Foundation and PATH, a nonprofit health organization, to develop
For many people around the world, the COVID-19 pandemic was an eye-opening event that revealed the dangers and inadequacies of the world’s global health systems. However, for other people, outbreaks of epidemic diseases might be more of a lived reality. On the continent of Africa, many know a certain geographic region in sub-Saharan Africa as the “meningitis belt.” These 26 countries face the dangers of meningitis more than other places around the world, and the outbreak of the COVID-19 pandemic delayed the vaccination of the MenAfriVac meningitis vaccine to 50 million children in these countries. African governments collaborated with the World Health Organization (WHO), the Bill and Melinda Gates Foundation and PATH, a nonprofit health organization, to develop 