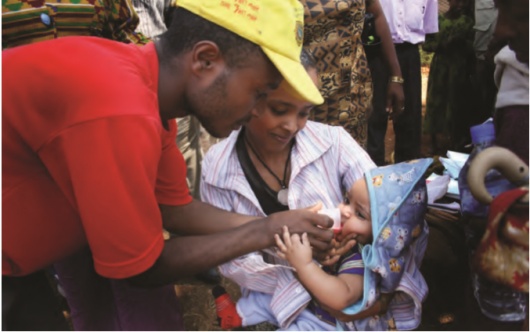
The Democratic Republic of the Congo (DRC) is one of Africa’s largest countries. With an especially high poverty rate, approximately 60 million people live on less than $2.15 a day. Vaccination struggles worsen living conditions by driving up child mortality. However, the government has been steadfast in improving the quality and quantity of vaccinations in the DRC and has doubled down on vaccine programs to improve the country.
The Democratic Republic of the Congo (DRC) is one of Africa’s largest countries. With an especially high poverty rate, approximately 60 million people live on less than $2.15 a day. Vaccination struggles worsen living conditions by driving up child mortality. However, the government has been steadfast in improving the quality and quantity of vaccinations in the DRC and has doubled down on vaccine programs to improve the country.
The Gavi Alliance
A key barrier to vaccinations in the DRC is cost; having resources to cover the massive 2 million square kilometers the country spans is a tall order. The Gavi Alliance, a global NGO championing vaccine equity, has donated a staggering $60 million to the DRC through its equity accelerator fund. The goal of the donations is to reduce the number of “zero-dose” children in the DRC. Zero-dose is a term that refers to the number of children who have received no vaccinations whatsoever, and the fund plans to reduce the number of these kids by 35% within only three years.
A focal point of Gavi’s mission is promoting equity. Their funds in the DRC will focus on creating Civil Society Organizations that will track zero-dose numbers, as well as tackle gender equity and vaccine inequalities throughout the country. The massive relief effort targets 11 provinces that harbor 74% of zero-dose cases. The DRC currently maintains one of the highest unvaccinated rates for children — 700,000 — and Gavi hopes to shatter that with “innovation and targeted support, [to]reach zero-dose children, and ensure that the most marginalized communities are no longer left behind,” according to Thabani Maphosa, Managing Director of Country Programmes Delivery at Gavi.
Maksho Plan
Another stride for vaccinations in the DRC is building on successes made before the COVID-19 pandemic. The Maksho Plan is another target vaccine program that has aimed to reduce the number of zero-dose children, increasing vaccination rates by 27% in 2019. During the pandemic, however, its impacts diminished, with national vaccination falling by 9%.
In response, the government has initiated the Maksho Plan 2.0 to further fight the zero-dose crisis. By 2023 they have brought the national vaccination coverage back to 45%. This increase is a substantial victory for the country and shows great signs of global health improvements in the future. The Maksho Plan and the DRC’s Ministry of Health have set their sights on increasing the percentage of vaccinated children to 75% by 2027.
Powerful Polio Efforts
Although countries like the United States have eradicated polio, it is still a very present threat to vaccinations in the DRC. Specifically, the polio strain noPV2 is the culprit of the DRC’s problems and is also the most common form of polio throughout Africa. Fortunately, because the disease has been successfully eradicated in other countries, the primary method of paving success is simply strong vaccine rollouts.
On June 1, 2023, the country launched its first large-scale effort on polio vaccinations. The force was a three-day wave across 20 DRC provinces, reaching 17 million children 5 and under. Half of all Africa’s polio cases are in the DRC, so this onslaught vaccine effort is a massive move to empower the public health of their citizens. The country is continuing its plans with a new mobile app that can track vaccines, health care workers, the quality of the campaign and other vital data for making improvements.
A Bright Future
The combined efforts from the Gavi Alliance, the Maksho Plan and the government’s Polio campaign have set vaccinations in the DRC on a fast track to success. The country has positioned itself to reach its milestone goals for reducing its zero-dose population. The DRC’s strategic vaccine endeavors may become a blueprint for other countries hoping to improve the health of their people.
– Aditya Arora
Photo: Flickr





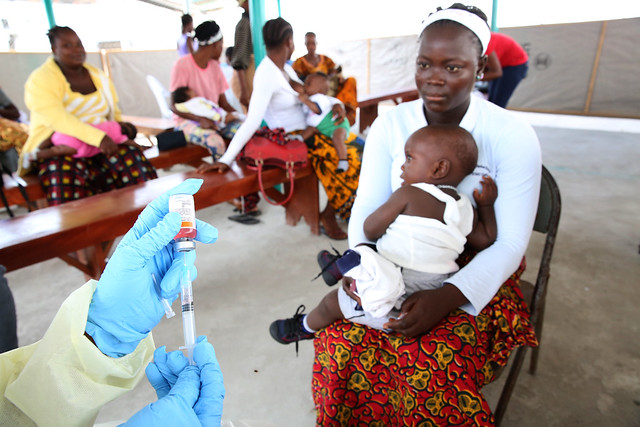 The Global Alliance for Vaccines and Immunization (Gavi) is a global organization whose goal is to create
The Global Alliance for Vaccines and Immunization (Gavi) is a global organization whose goal is to create