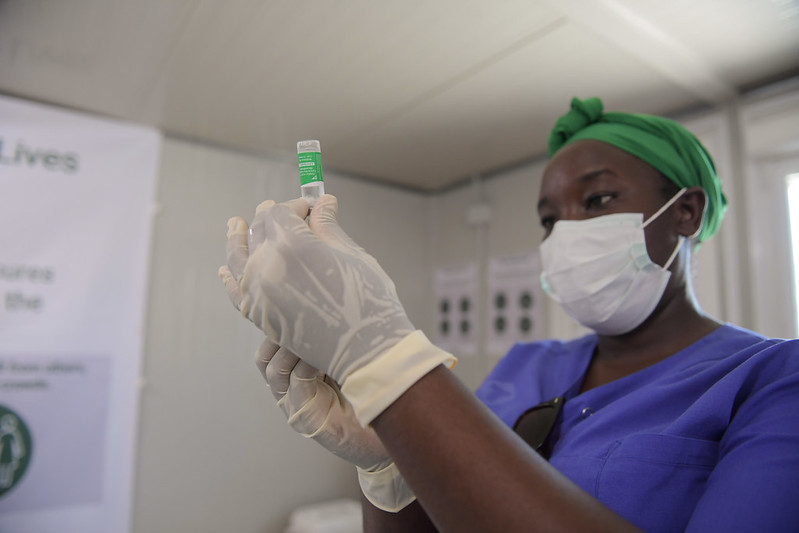
 The World Health Organization’s (WHO) 2025 tracking report on Universal Health Coverage (UHC) indicates that several challenges persist in the complex process of health care reform. However, improvements have been made across the board toward UHC in most countries and further progress is possible.
The World Health Organization’s (WHO) 2025 tracking report on Universal Health Coverage (UHC) indicates that several challenges persist in the complex process of health care reform. However, improvements have been made across the board toward UHC in most countries and further progress is possible.
Universal Health Coverage: Goals and Challenges
Universal Health Coverage has been recognized as an important component of the 2015 Sustainable Development Goals (SDGs), a set of 17 goals adopted by United Nations (U.N.) member states for attainment by 2030. SDG 3 aims to ensure health and promote well-being for all people. According to the report, “UHC means that all people receive the health services they need without facing financial hardship.”
According to the WHO, as of 2021, 4.5 billion people (more than half of the global population) were not covered by essential health services. Even those who do receive essential coverage may experience financial hardship when using it, partly due to high out-of-pocket (OOP) costs. These costs are often catastrophic for households already struggling with or threatened by poverty.
According to the 2025 monitoring report, low-income countries have made the fastest progress towards UHC. However, these countries still have the furthest to go before reaching UHC goals. Low and middle-income countries are especially vulnerable to noncommunicable diseases (NCDs), which, according to the WHO, pose a significant threat to health in countries without adequate health care.
Common NCDs include cardiovascular diseases, cancers and chronic respiratory diseases. According to the WHO estimates, nearly three-quarters of NCD deaths occur in low and middle-income countries.
Progress Persists
Several countries have made significant progress toward UHC. A 2023 article in Exemplars in Global Health (EGH) reports on the steps countries such as Thailand, Ethiopia and Ghana have taken toward achieving UHC. These case studies suggest that adopting UHC is only one step toward equitable, affordable and accessible health care for all.
They underscore the importance of an integrative, holistic approach when reforming an entire health care system.
Thailand’s Investments in Primary Health Care Pay Off
Thailand’s journey with health care reform has illustrated the importance of strengthening primary health care systems alongside the adoption of a UHC program. When the country launched its UHC program in 2002, it responded to rising demand by investing heavily in its public health workforce, sharply increasing the number of doctors, midwives and nurses.
WHO Director-General Dr. Tedros Adhanom Ghebreyesus has emphasized the central role of primary health systems (PHS) in achieving UHC. He says investments in PHS are “the most inclusive, equitable and efficient path to UHC.” PHS can improve the distribution of care across both rural and urban areas.
In contrast, heavy investment in hospital-based care can concentrate health workers in cities. A collaborative study by the World Bank and the Government of Japan supports this finding. The study surveyed 11 countries at different stages of progress toward UHC.
It found that progress is typically incremental and highly context-specific, with shared challenges and a need for sustained political commitment and tailored policies to expand coverage.
Ethiopia Commits to Equity in Health Care
Ethiopia’s gains toward UHC have come with a commitment to equity, as reflected in its recognition of women’s specific health care needs. This has been realized through the development and expansion of services and resources. These include family planning, prenatal care, birthing facilities and qualified women’s health professionals such as birth attendants and obstetric care providers.
These areas of care were a key focus of the country’s 2003 Health Extension Program. According to the World Bank, the program has played a central role in the country’s strong progress in improving health outcomes and expanding coverage.
Decreasing OOP Costs in Ghana
Ghana offers another example of progress toward UHC. The country’s National Health Insurance Scheme (NHIS), which is heavily subsidized by taxes and a national health insurance levy, makes care free at the point of service. According to the EGH, NHIS has reduced OOP costs for insured individuals.
However, the scheme covers less than 70% of the population. The poorest households remain the most vulnerable to OOP expenses that can be financially catastrophic. The article also notes that medical bills are not the only factor straining households.
Other costs, such as transportation, diagnostic tests and lost income from time away from work, can also undermine a family’s financial stability and overall well-being.
Final Remarks
These case studies show what health care reform can achieve when there is a commitment to equitable care, practical and integrated approaches and a willingness to adopt and adapt new strategies.
– Emma Kelsey
Emma is based in St. Paul, MN, USA and focuses on Good News and Global Health for The Borgen Project.
Photo: Unsplash
 On February 1, 2025, Rwanda launched a mission entitled Mission 2027, where they are trying to sustain a goal of reducing the number of cases of cervical cancer in women in Rwanda. This goal aims to reach fruition three years ahead of the World Health Organization’s (WHO) mission of 2030.
On February 1, 2025, Rwanda launched a mission entitled Mission 2027, where they are trying to sustain a goal of reducing the number of cases of cervical cancer in women in Rwanda. This goal aims to reach fruition three years ahead of the World Health Organization’s (WHO) mission of 2030. South-South cooperation, which offers solutions through solidarity, is key to
South-South cooperation, which offers solutions through solidarity, is key to 
 Within Europe, the
Within Europe, the  Lebanon’s medical system faces immense strain as ongoing conflict with Israel has led to widespread damage to health care facilities and personnel. Israeli airstrikes across the country—particularly in southern
Lebanon’s medical system faces immense strain as ongoing conflict with Israel has led to widespread damage to health care facilities and personnel. Israeli airstrikes across the country—particularly in southern  Children with disabilities face
Children with disabilities face  Approximately 1.2 billion people live in acute, multidimensional poverty
Approximately 1.2 billion people live in acute, multidimensional poverty  At the end of 2023,
At the end of 2023,