 Limited health care infrastructure, economic vulnerability and heavy reliance on external humanitarian aid make the fight against HIV/AIDS in Comoros fragile. While HIV prevalence remains low, progress depends largely on donor-funded programs. Inconsistent and short-term funding threatens to reverse gains in prevention, treatment access and health system resilience. Sustained funding for HIV/AIDS in Comoros is essential to ensure long-term prevention, uninterrupted treatment and national health stability.
Limited health care infrastructure, economic vulnerability and heavy reliance on external humanitarian aid make the fight against HIV/AIDS in Comoros fragile. While HIV prevalence remains low, progress depends largely on donor-funded programs. Inconsistent and short-term funding threatens to reverse gains in prevention, treatment access and health system resilience. Sustained funding for HIV/AIDS in Comoros is essential to ensure long-term prevention, uninterrupted treatment and national health stability.
HIV/AIDS in Comoros: A Fragile Success
HIV prevalence in Comoros remains below 1%, one of the lowest rates in sub-Saharan Africa. This success is largely due to early prevention strategies, cultural factors and donor-supported health programs. However, limited domestic health financing means that HIV/AIDS services depend heavily on external support for antiretroviral treatment (ART), testing services and public awareness campaigns. Any reduction in funding risks service disruption, increased transmission and setbacks to national health goals. Donor-supported programs have included nationwide HIV awareness campaigns, voluntary counseling and testing services and integration of HIV services into primary health care, all of which have contributed to maintaining low prevalence levels. Here is why sustained funding matters.
Continuity of Treatment
HIV is a lifelong condition with no cure and requires continuous treatment with antiretroviral drugs to suppress the virus and protect the immune system. According to the World Health Organization (WHO), uninterrupted ART significantly reduces HIV-related deaths and prevents drug resistance. Funding interruptions can lead to medication shortages, treatment gaps and declining health outcomes. Sustained funding for HIV/AIDS in Comoros ensures consistent patient monitoring, reliable medication supply and effective long-term care.
In Comoros, antiretroviral treatments are largely financed internationally, particularly grants from the Global Fund. According to UNAIDS, this external supply creates challenges such as supply chain delays, limited laboratory capacity and difficulties to provide a consistent patient follow-up across the islands. Sustained funding for HIV/AIDS in Comoros ensures consistent patient monitoring, reliable medication supply and effective long-term care.
Prevention and Education
Prevention and education programs are critical to maintaining low HIV prevalence in Comoros. One major example is the national prevention of mother-to-child transmission (PMTCT) program, supported by international partners such as UNICEF and WHO, which provides testing, treatment and counseling to pregnant women living with HIV; as a result, HIV prevalence among pregnant women stands at an exceptionally low level and infants born to HIV-positive mothers have consistently tested HIV-negative under this initiative.
Existing initiatives include community-based awareness campaigns supported by UNAIDS and the Global Fund, HIV testing and counseling services and outreach programs targeting young people and women. International assistance has supplied critical testing equipment and strengthened health worker training, helping expand access to HIV information and services. These programs promote safe practices, reduce stigma and encourage early testing. Long-term funding allows these initiatives to operate consistently and expand into underserved communities, particularly in rural areas.
Strengthening Health Systems
Efforts are underway to broaden health system improvements in Comoros. Investments have supported clinic infrastructure, trained health care workers and strengthened disease surveillance systems. However, challenges remain, including shortages of medical staff, limited laboratory capacity and unequal access to care between urban and rural regions. These weaknesses increase vulnerability to HIV transmission and hinder treatment access.
In Comoros, HIV/AIDS-related investments have contributed to improved primary health facilities and health worker training, but the country continues to face shortages of medical personnel and limited diagnostic infrastructure, particularly outside urban areas. According to the World Bank, stronger health systems improve economic resilience and reduce poverty in developing countries.
Solution in Action: The Global Fund
Established in 2002, the Global Fund has played a key role in supporting HIV/AIDS programs in Comoros. The Global Fund is one of the main external financiers of HIV/AIDS programs in Comoros, supporting HIV treatment and prevention efforts in collaboration with national health authorities. By financing antiretroviral therapy, HIV testing and health system strengthening, the organization has expanded access to essential services.
According to the Global Fund, its investments support the delivery of HIV services across the country, demonstrating how sustained international funding strengthens national health capacity. In 2023, countries supported by the Global Fund reported that approximately 25 million people were on antiretroviral therapy, and 53.8 million HIV tests were conducted through its investments, reaching millions with prevention services. While these figures reflect global outcomes, they illustrate the scale of support provided to countries like Comoros.
Poverty and HIV/AIDS in Comoros
Poverty remains a significant challenge in Comoros, where a large portion of the population lives below the national poverty line. Using the international poverty line of $3.65 per day, about 39.5% of Comorians lived in poverty in 2023, reflecting persistent economic hardship that constrains access to essential services like health care, education and transportation. In Comoros, long distances to health facilities, high out-of-pocket costs for care and shortages of trained health workers make it difficult for poor households to obtain HIV testing and treatment services, contributing to health inequalities. People living in poverty are also more vulnerable to poor health outcomes due to malnutrition and limited medical access. Addressing HIV/AIDS through sustained funding helps reduce these inequalities and supports broader poverty reduction efforts.
The Role of International Support
International support remains vital to sustaining HIV/AIDS programs. Comoros participates in regional HIV response efforts coordinated by UNAIDS and partners, such as Indian Ocean Island forum meetings aimed at strengthening prevention and treatment planning, demonstrating the active role of international support in shaping the country’s HIV strategy. Donor countries and multilateral institutions help bridge funding gaps while the government gradually strengthens domestic health financing. Sustained funding aligns with global commitments to end AIDS as a public health threat by 2030 and ensures that small island developing states like Comoros are not left behind.
Conclusion
The fight against HIV/AIDS in Comoros is about securing long-term public health and economic stability. Sustained funding ensures uninterrupted treatment, effective prevention strategies and stronger health systems. Programs supported by the Global Fund and other international partners show that long-term investment expands access to ART, increases testing in rural communities and reduces health disparities. With predictable and sustained funding, Comoros can continue to maintain low HIV prevalence, improve health outcomes and support sustainable development.
– Numahaiseta Sillah Tunkara
Numahaiseta is based in Duisburg, Germany and focuses on Technology and Politics for The Borgen Project.
Photo: Flickr
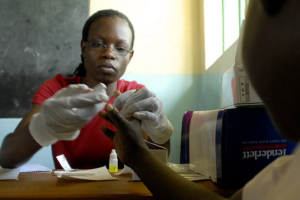 Malaria prevention in sub-Saharan Africa remains a critical global health priority. Despite significant progress over the past two decades, malaria continues to affect countries across the region disproportionately. Expanding prevention efforts is essential to saving lives, strengthening economies and reducing poverty.
Malaria prevention in sub-Saharan Africa remains a critical global health priority. Despite significant progress over the past two decades, malaria continues to affect countries across the region disproportionately. Expanding prevention efforts is essential to saving lives, strengthening economies and reducing poverty. Limited health care infrastructure, economic vulnerability and heavy reliance on external humanitarian aid make the fight against HIV/AIDS in Comoros fragile. While
Limited health care infrastructure, economic vulnerability and heavy reliance on external humanitarian aid make the fight against HIV/AIDS in Comoros fragile. While 


 The landlocked country of Tajikistan has for years had
The landlocked country of Tajikistan has for years had  The number of people
The number of people 
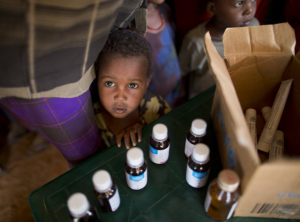 Somalia, a large country nestled in the Horn of Africa, is one of many developing countries affected by the AIDS epidemic, though not to the extent of other areas within sub-Saharan Africa. Though Somalia notes a relatively low prevalence rate of HIV/AIDS at
Somalia, a large country nestled in the Horn of Africa, is one of many developing countries affected by the AIDS epidemic, though not to the extent of other areas within sub-Saharan Africa. Though Somalia notes a relatively low prevalence rate of HIV/AIDS at 
