 Home to nearly 25% of the global population, South Asia is one of the world’s most populous yet vulnerable regions, facing extensive health disparities due to poverty, limited health care infrastructure and high disease burdens. South Asia has the second-highest number and proportion of the world’s extremely poor at a staggering 33.4%. In response, countries like India, Pakistan and Bangladesh have launched targeted health initiatives to address these ongoing challenges, especially for marginalized populations.
Home to nearly 25% of the global population, South Asia is one of the world’s most populous yet vulnerable regions, facing extensive health disparities due to poverty, limited health care infrastructure and high disease burdens. South Asia has the second-highest number and proportion of the world’s extremely poor at a staggering 33.4%. In response, countries like India, Pakistan and Bangladesh have launched targeted health initiatives to address these ongoing challenges, especially for marginalized populations.
Bangladesh
In Bangladesh, mobile health clinics are reaching remote communities, providing essential health care that would otherwise be inaccessible. BRAC, one of the world’s largest NGOs, has partnered with the government to deploy these clinics across rural areas, delivering crucial services to more than 20 million people annually. In addition to general health care, these mobile clinics offer antenatal and postnatal care, vaccinations and nutrition counseling, all of which are critical in a country where approximately 60% of the population lives in rural areas without easy access to health care facilities.
The Shasthya Shebika initiative, one of BRAC’s standout programs, trains local women to serve as health workers. With more than 50,000 Shasthya Shebikas operating in rural communities, this program reaches more than 80 million people across Bangladesh. The initiative has been shown to reduce maternal mortality in the areas it serves, highlighting the effectiveness of community-based health care support in reducing life-threatening childbirth complications.
Pakistan
In Pakistan, vaccination efforts have led to significant reductions in preventable diseases. Polio, once a widespread threat, is now close to being eradicated due to a massive vaccination campaign launched in partnership with UNICEF and the World Health Organization (WHO). Since 1988, polio cases in Pakistan have dropped by more than 99%—from thousands annually to just a handful in recent years. In 2021, the campaign vaccinated more than 40 million children under 5 across the country, illustrating the reach and impact of sustained immunization efforts.
Pakistan’s Sehat Sahulat Program, a health care financing initiative introduced in 2015, provides health care cards to families earning less than $2 per day. The program currently covers more than a million families, providing them with up to $6,000 annually for medical expenses, including surgeries, maternal health services and emergency care. Studies reveal that households participating in the program are more likely to seek medical care early, reducing disease progression and associated health care costs.
India
In India, where infant mortality and malnutrition are significant challenges, programs like Saans and Poshan Abhiyaan are making measurable progress. The Saans Initiative, launched by the Ministry of Health and Family Welfare, trains community health workers to perform neonatal resuscitation, reducing neonatal mortality rates in rural and underserved areas. Studies reveal that trained health workers can reduce neonatal deaths by up to 20% in resource-limited areas, a statistic supported by Saans data from states like Madhya Pradesh, where the program is heavily implemented.
On the nutrition front, Poshan Abhiyaan (National Nutrition Mission) has been a cornerstone in India’s fight against child malnutrition. Launched in 2018, this program targets stunting, wasting and anemia among children under 5 and women of reproductive age. Since its inception, the mission has reached more than 80 million people across India. Data from the National Family Health Survey reveals a 6% reduction in stunting and a 2% reduction in wasting among children between 2016 and 2020, attributed in part to Poshan Abhiyaan’s focus on community-based nutrition programs, counseling and distribution of fortified foods.
Looking Ahead
The success of health initiatives in South Asia hinges on strong partnerships, leveraging local expertise and international resources to drive sustainable, large-scale impact. Collaborations between BRAC and Bangladesh’s Ministry of Health, Pakistan’s Sehat Sahulat with GIZ and India’s Poshan Abhiyaan with UNICEF and the World Bank have empowered millions, reducing maternal mortality, nearly eradicating polio and lowering childhood stunting rates. Together, these ongoing initiatives transform health access and quality of life for vulnerable populations, creating a foundation for lasting health improvements across South Asia.
– Irtija Ahmad
Irtija is based in Slough, Berkshire, UK and focuses on Global Health for The Borgen Project.
Photo: Flickr
 Access to health care poses a significant
Access to health care poses a significant 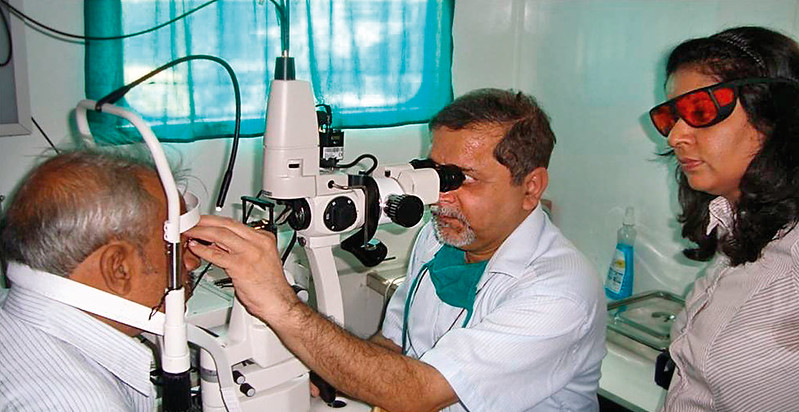
 While acknowledging the need for continued progress worldwide, it’s also crucial to recognize significant advances. Moreover, the year 2023 was noteworthy for global health achievements, particularly marking strides away from the COVID-19 pandemic. Here’s to celebrating six notable global health advancements from 2023.
While acknowledging the need for continued progress worldwide, it’s also crucial to recognize significant advances. Moreover, the year 2023 was noteworthy for global health achievements, particularly marking strides away from the COVID-19 pandemic. Here’s to celebrating six notable global health advancements from 2023. Southeast Asia, a region known for its vibrant cultures and dynamic economies, is also home to some of the most innovative health care transformations in the world. Among these, the rise of e-health startups in Southeast Asia stands out as a critical development, leveraging technology to bridge significant gaps in health care services. Furthermore, this surge reflects a broader trend of digitalization in the health care sector, driven by the urgent need to improve access, affordability and the quality of health care services across diverse populations.
Southeast Asia, a region known for its vibrant cultures and dynamic economies, is also home to some of the most innovative health care transformations in the world. Among these, the rise of e-health startups in Southeast Asia stands out as a critical development, leveraging technology to bridge significant gaps in health care services. Furthermore, this surge reflects a broader trend of digitalization in the health care sector, driven by the urgent need to improve access, affordability and the quality of health care services across diverse populations.


 When it comes to health care, video games do not typically come to mind. There has been some research about the positive impacts on the brain, or scientists developing smaller research games. While this suggests positive signs, the overlap between video games and science is not well-known. Nevertheless, here are three video games that aid global health.
When it comes to health care, video games do not typically come to mind. There has been some research about the positive impacts on the brain, or scientists developing smaller research games. While this suggests positive signs, the overlap between video games and science is not well-known. Nevertheless, here are three video games that aid global health. The nation of Australia suffers from the highest rates of cancer in the world, but, the disease takes a significant toll on the disadvantaged and rural residents in particular. Impoverished and disadvantaged Australians are
The nation of Australia suffers from the highest rates of cancer in the world, but, the disease takes a significant toll on the disadvantaged and rural residents in particular. Impoverished and disadvantaged Australians are 