 Homelessness and mental health are problems that exist around the world, developed and undeveloped countries alike. Among homeless youth in East Asia and Southeast Asia, mental health is a massive issue. These youth typically become homeless due to past abuse, and usually experience more while on the streets; past research has shown that homeless youth are highly susceptible to sexual exploitation and prostitution.
Homelessness and mental health are problems that exist around the world, developed and undeveloped countries alike. Among homeless youth in East Asia and Southeast Asia, mental health is a massive issue. These youth typically become homeless due to past abuse, and usually experience more while on the streets; past research has shown that homeless youth are highly susceptible to sexual exploitation and prostitution.
This demographic of homeless youth reports high rates of mental health issues, such as depression, PTSD, bipolar disorder and suicidal ideation, with suicide being their leading cause of death, and 80% of the population having reported attempting suicide at some point. To cope with these issues, many turn to substance abuse and other maladaptive coping mechanisms. 66.7% report drinking problems, and 77.8% report smoking problems.
Causes of Homelessness
There are various reasons why youth become homeless in the first place. It is worth mentioning that one primary cause of poverty in the East Asian Pacific region is natural disasters. Natural disasters like earthquakes and tsunamis affect East and Southeast Asia more than most other regions in the world, making them a significant and notable contributor to homelessness that might not necessarily apply or apply as much to other regions around the globe, according to a 2024 article.
Poverty can cause stress and subsequent dysfunction in the home, driving children and young people away. A 2024 article found that parental abuse was the most common reason (40.7%) for leaving home, especially from fathers. General family conflict follows at 29.6%.
Cultural Differences
Treating these problems requires understanding and accommodating the differences in cultural attitudes between Eastern and Western societies. Due to the way Eastern cultures raise kids to view themselves, their obligation to and role within family and the way they view mental health itself, means that Western mental health techniques do not always transfer or have the same result.
For example, Western programs tend to emphasize working with direct service providers and place a lot of value on individual autonomy. Conversely, services and government interventions in the East Asian Pacific regions might put more emphasis on family and community support.
Few components of culture influence mental health and responses to mental health treatment. The first is emotional expression: depending on what level of emotional outburst or emotional behavior is considered acceptable in a given culture, it will be easier or harder to identify when a person needs help. The second and likely most influential element is shame: many cultures, especially Asian cultures, see mental illness as something shameful or born out of weakness.
Individuals may be hesitant to seek treatment because it means admitting to themselves and to a mental health professional that they are struggling. Individuals may also be reluctant to interact with a mental health professional because of the third element, “power distance,” according to the Frontiers in Public Health. Regulations on mental health treatment and the power given to mental health professionals vary from country to country, having varied implications about autonomy and the power dynamic within a therapeutic relationship.
Results
A 2024 article revealed the results of eight studies conducted throughout Malaysia, South Korea and the Philippines. These studies researched the impacts of various mental health interventions on homeless youth, including art therapies, cognitive behavioral therapy (CBT), life skills education (LSE) and government services.
A Philippines-based study found visual art and poetry psychotherapies to be effective for abused adolescents in reducing symptoms of PTSD and depression, measured via Child Report on Posttraumatic Symptoms (CROPS) and Self-Rating Depression Scale (SDS). It was noted that art therapies seemed to also help empower homeless youth to engage actively in their own treatment.
A study on CBT implemented in South Korea measured impacts on depression, self-efficacy, and self-esteem. While the treatment resulted in increased self-efficacy and a significant decrease in depression, there appeared to be no significant difference in self-esteem pre- and post-test. LSE treatment, however, was successful in increasing self-esteem, as well as decreasing anxiety, depression and stress, according to a study out of Malaysia.
Closing Thoughts
While these mental health interventions have appeared to be successful, one of the key takeaways is that it is difficult to treat this demographic when there is no universally accepted definition of homelessness. Every study and every country uses different definitions, which leaves large gaps in understanding both the nuance and variation within the “homeless” experience and the actual overall figures of the demographic. Whether or not an individual fits within a jurisdiction’s given definition of homelessness may determine whether or not mental health and homeless services are provided to them; this makes the varying definitions of homelessness a possible barrier to mental health services.
– Sandhya Mathew
Sandhya is based in Los Angeles, CA, USA and focuses on Global Health for The Borgen Project.
Photo: Pixabay

 Heart diseases are a very common problem in Pakistan.
Heart diseases are a very common problem in Pakistan. 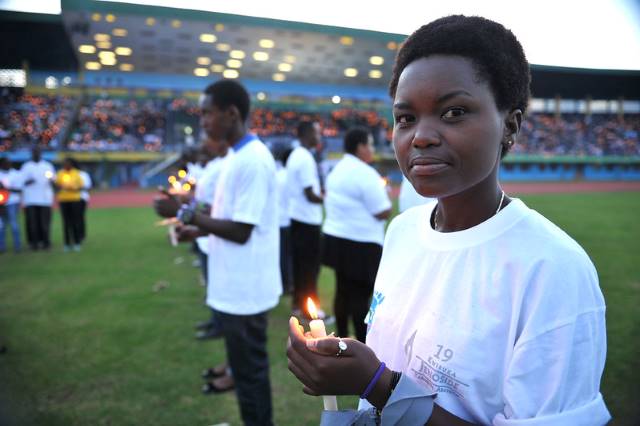 Rwanda is a small country in sub-Saharan Africa. Rwanda has struggled to become a stable country economically and politically since it became independent in 1962. As a developing country, Rwanda is still trying to develop its healthcare system. With years of conflict and instability, people especially struggle with mental health in Rwanda.
Rwanda is a small country in sub-Saharan Africa. Rwanda has struggled to become a stable country economically and politically since it became independent in 1962. As a developing country, Rwanda is still trying to develop its healthcare system. With years of conflict and instability, people especially struggle with mental health in Rwanda.

 Depression is one of the
Depression is one of the  Almost ten years after the global financial crisis, the cost of living in Greece has continued to climb, while wages and available jobs have dropped considerably. This unceasing contraction of the Greek economy has led to a sharp increase in the percentage of the population living in
Almost ten years after the global financial crisis, the cost of living in Greece has continued to climb, while wages and available jobs have dropped considerably. This unceasing contraction of the Greek economy has led to a sharp increase in the percentage of the population living in 

