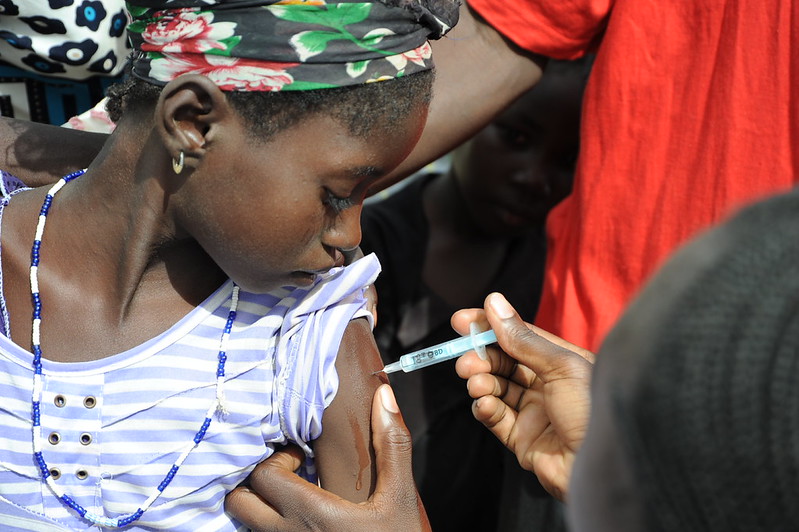
 Many people in Africa cannot get the care or medicines they need, or they must pay for treatments themselves, causing nearly 11 million low-income Africans to fall into poverty every year. Determined to rectify this inequitable situation, participants at the 2025 Conference on Public Health held in Durban, South Africa, endorsed a pledge stating that Africa will begin to manufacture, regulate, and procure its medical items internally. Known as The Durban Promise for African health sovereignty, the assertion aims to promote health care equity by lowering costs and creating millions of jobs for its citizens, helping to alleviate poverty and provide universal health coverage to all Africans.
Many people in Africa cannot get the care or medicines they need, or they must pay for treatments themselves, causing nearly 11 million low-income Africans to fall into poverty every year. Determined to rectify this inequitable situation, participants at the 2025 Conference on Public Health held in Durban, South Africa, endorsed a pledge stating that Africa will begin to manufacture, regulate, and procure its medical items internally. Known as The Durban Promise for African health sovereignty, the assertion aims to promote health care equity by lowering costs and creating millions of jobs for its citizens, helping to alleviate poverty and provide universal health coverage to all Africans.
The Need for African Health Sovereignty
Africa currently imports about 70% of its medicines, 90% of its medical devices, and 99% of its vaccines. This drives up costs and limits medical treatment accessibility for many Africans. Adding more urgency to the situation, global health funding in Africa has declined 70% since 2021. Significant cuts to the USAID and reduced contributions from European donors seemed to make universal health care coverage (UHC) for Africa even less attainable.
However, African leaders anticipated the reductions and were actively seeking alternative sources of health care subsidies. As a result, China pledged $50 billion to support Africa’s health care program, funding that has accelerated the building of hospitals and clinics. Indeed, with significant financing, the Durban Promise is on the way to becoming a reality, bringing universal health care coverage within reach.
The Road to UHC
African governments have been working towards universal health care coverage for more than 20 years, but have faced significant obstacles. The Abuja Declaration of 2021 asserted that 15% of African national budgets should be allocated for health care, though many African countries still spend less than half that amount in the medical arena.
In 2023, African leaders signed The Lusaka Agenda, compelling governments to meet Abuja obligations and to implement actions that would lower the cost of medicine. However, this agenda was not fully successful due to challenges with domestic financing. With minimal results from these initial affirmations, in October 2025, African governments signed The Durban Promise, a roadmap for African health sovereignty and security that suggests an innovative medical financing structure to move Africa’s health care goals forward.
The 2025 G20 Summit
The annual G20 summit, which the African Union joined in 2023, brings together developed and emerging economies to address urgent global issues. The 2025 summit, held in Johannesburg, South Africa, marked the first time the assembly met on African terrain. The agenda from the South Africa’s President Cyril Ramaphosa discussed the challenges of developing nations, which include the pressing issue of health insecurity. Ramaphosa’s compelling arguments led to increased funding from the World Health Organization and a Global Health Security Pact for equitable vaccines and sharing of data during global health emergencies. The pact further addresses African health security and the goals of the Durban Promise.
The Presidential Declaration
At the 39th African Union Summit in Addis Ababa, Ethiopia, in February 2026, countries made the commitment of the Durban Promise, according to AfricaCDC. The Presidential Declaration on Advancing Local Manufacturing of Health Products in Africa was issued with the objective that the African continent will produce 60% of medical products internally by 2040. The declaration includes two key strategies led by the African Center for Disease Control (CDC) focusing on securing the goal of health autonomy: The Platform for Harmonized African Health Products Manufacturing (PHAHM) and The African Pooled Procurement Mechanism (APPM).
By creating a single health product market, the PHAHM will help align regulatory and manufacturing policies across the African Union. The APPM could enable African countries to leverage their joint bargaining power to make the market more predictable and desirable for suppliers, leading to supply security. Together, these approaches can help African health care to thrive.
Outlook for African Medical Sovereignty
There is much to do in order to achieve the goal of producing 60% of medical products on the African continent in less than 15 years. As daunting a task as it may be, with a thoughtful, well-executed plan and targeted efforts, the result can be a robust health program that will contribute to regional income and poverty reduction as articulated in The Durban Promise.
– Debbie Barto
Debbie is based in Monroe, WA, USA and focuses on Technology and Global Health for The Borgen Project.
Photo: Flickr
 A
A
 Nano enzymes (nanozymes) are an
Nano enzymes (nanozymes) are an 

 HIV/AIDS has been one of the most taboo diseases to date, with many having negative attitudes and beliefs about people who have it. Harmful stereotypes about HIV/AIDS have prevented those who need help from getting the proper treatment they deserve.
HIV/AIDS has been one of the most taboo diseases to date, with many having negative attitudes and beliefs about people who have it. Harmful stereotypes about HIV/AIDS have prevented those who need help from getting the proper treatment they deserve.  India is the most populous country in the world,
India is the most populous country in the world, 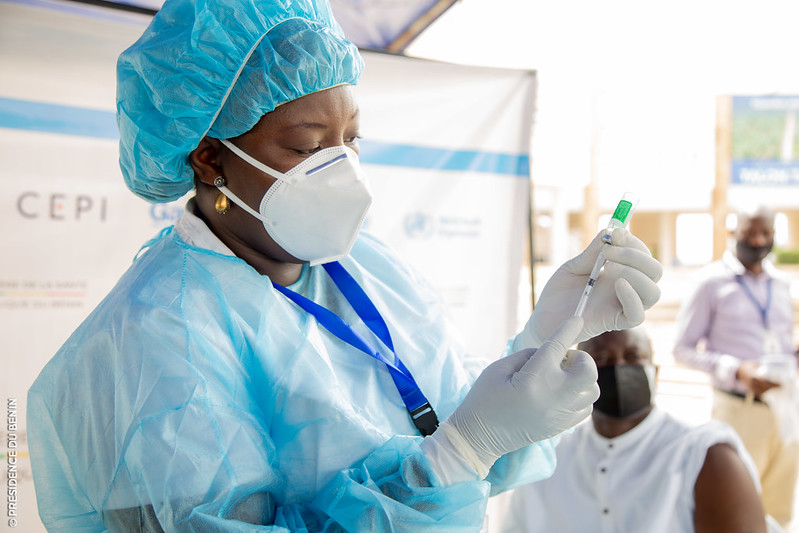 Nigeria is
Nigeria is  With a
With a 