Vaccines in Developing Countries: Challenges and Solutions
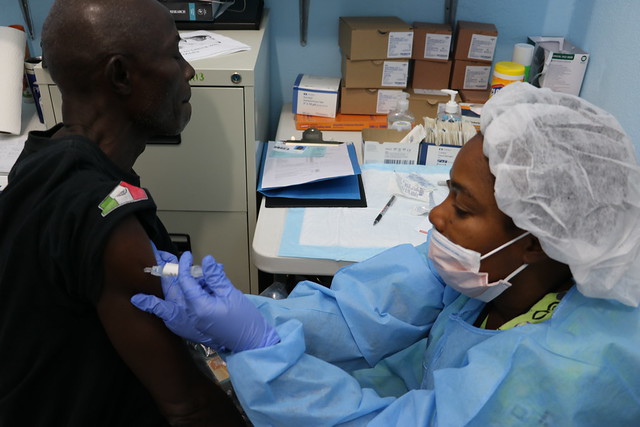 How much can the world really rely on vaccines as a cure to disease? For many impoverished communities, the jury is still out; many recent studies show that vaccines in developing countries are more ineffective than those in developed, high-income nations.
How much can the world really rely on vaccines as a cure to disease? For many impoverished communities, the jury is still out; many recent studies show that vaccines in developing countries are more ineffective than those in developed, high-income nations.
However, developing countries are at greater risk for all infectious diseases than developed countries. The World Health Organization (WHO) documented that the “total number of healthy life years lost per capita was 15-times higher in developing countries than in developed countries.” In addition to this imbalance, vaccines in developing countries also threaten these nations with ineffective treatment. Due to the many factors that impact disease, it is difficult to pinpoint specific causes behind vaccine acceptance or denial. However, the health effects of poverty contribute to the reasons why vaccines in developing countries are often ineffective.
How Poverty Increases Sickness
Poverty is a health epidemic. In 2008, PBS aired an original docu-series called “Unnatural Causes” that outlined the ways diseases disproportionately affect poor and marginalized groups. The show posed one overarching, famous question: “Is inequality making us sick?” In the assessment of vaccine effectiveness in rich versus poor countries, the creators of “Unnatural Causes” say the answer is yes.
A functioning immune system is largely responsible for an individual’s ability to make antibodies, the infection-fighting proteins developed via vaccines. Impoverished people often do not have high-functioning immune systems. This means that they cannot produce antibodies as well as their developed-nation counterparts.
Multiple factors contribute to the prevalence of ineffective immune systems in developing countries. The overpopulation and crowding common in low socioeconomic areas increase the risk of disease exposure. Pre-existing health conditions, resulting from vitamin deficiency and little clean water or sanitation, increase individual susceptibility to sickness. Further, unreliable health care places systemic, structural constraints on impoverished communities. In this way, poverty and disease continually reinforce each others’ negative effects.
Comparison Studies: Developed Nations vs. Developing Nations
Water-borne diseases, malaria, tuberculosis and HIV/AIDS continually afflict developing countries. They may be responsible for damaging people’s natural immunity, thus decreasing the likelihood of vaccine acceptance. Indeed, one study found that these diseases “may damage lymph node structures that are crucial to developing immunity after a vaccine.”
This study from the University of Minnesota compared Americans to Ugandans. Researchers discovered all the Ugandans had “significantly higher levels of inflammation in their bodies and a depleted supply of protective T cells.” In addition, the Ugandan’s lymph nodes (which help filter infections and respond to vaccines) were inflamed and scarred. None of the American participants had these issues. After administering a yellow fever vaccine to the Ugandan test subjects, researchers discovered a positive correlation. The more damaged their lymph nodes, the less likely it was for antibodies to form.
Another series of studies in Dhaka, Bangladesh discovered that a poor response to vaccines in developing countries could be correlated to the small intestinal bacteria endemic to low-income countries. Petri’s team surmised that “inflammation [in the intestine] could prevent vaccines from lingering in the gut and could keep the immune system from reacting to them.” The team also identified a similar issue with rotavirus vaccine response. In contrast, 98% of children in the developed world do not have complications after vaccination.
The Future of Vaccines
According to the World Bank, “nearly half of the world lives on less than $5.50 a day.” In addition, only 59 of the 195 countries in the world possess a Human Development Index (HDI) at or above 0.8, making them developed countries. This means that ineffective vaccination responses affect the majority of the world’s nations. Thus, the world needs a systemic change in public health to fix this issue. Studies in Bangladesh and Africa “are testing whether sanitation interventions such as installing hand-washing stations in rural homes” can relieve the gut inflammation thought to be causing poor responses to vaccination.
However, even though vaccines in developing countries are sometimes ineffective, routine vaccination for infants and children may help. Young children are less likely to have the long-term health effects responsible for ineffective responses to vaccines, with the exception of illnesses inherited from a mother’s womb. WHO estimates that approximately 70% of the 9 million deaths from children under five “could be prevented or treated with access to simple, affordable interventions,” including vaccines.
Vaccinating Children in Developing Countries
Still, the complicated relationship to vaccines in the developing world is palpable. One study in India found that there is only a 55% rotavirus vaccine efficacy rate in young children. However, India’s plan to make the rotavirus vaccination routine may “save 27,000 of the 78,000 young lives that infections claim every year.”
Thus, expanding coverage of vaccines in developing countries has proven successful in many cases. Various programs work to extend this success. Since 1990, WHO’s Expanded Programme on Immunization has helped decrease mortality rates among infants and children via vaccination. The Global Vaccine Alliance has also “vaccinated more than half a billion additional children since its founding in 2000,” often in developing countries. While routine vaccination is not a panacea, it helps prevent disease before long-term health issues develop.
Improving World Health
Obviously, this is a hefty challenge. Changing human response to vaccines will take years of improving sanitation and living conditions. In addition, developed countries often receive vaccines first and in larger quantities due to having more money. In the meantime, scientists and doctors are experimenting with speedier methods to the vaccine problem. Take mesalazine, a drug that treats the bowel inflammation preventing antibody response to vaccines. This drug could possibly treat unreliable oral vaccines for stomach illnesses. Recognizing the issue of vaccines in developing countries is the first steps in improving global health.
– Grace Ganz
Photo: Flickr
