What is Being Done for Human African Trypanosomiasis
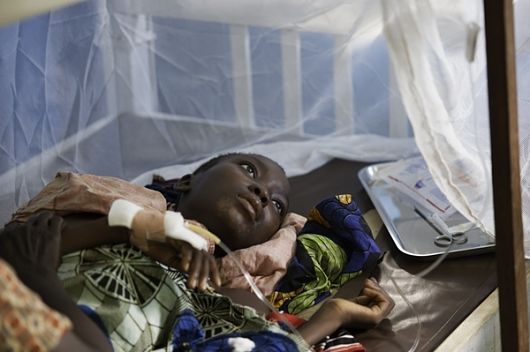
Human African Trypanosomiasis (HAT), also known as Sleeping Disease, is prevalent in Sub-Saharan Africa, affecting rural, poverty-stricken populations with close to 10,000 new cases each year. There are 2 strands of the disease: East African Trypanosomiasis and West African Trypanosomiasis. Both strands are only spread in rural Africa via the bite of tsetse flies and cause similar symptoms, but the incubation periods and medications used are slightly different.
A tsetse bite infects the patient with a parasite, which then lives in the host’s lymphatic system and blood stream. There is also a chance that a pregnant woman can pass the infection on to her child. HAT can cause headaches, fever, weakness, joint pain, stiffness and irregular sleep patterns in its first stages. When the infection advances and crosses over into the host’s nervous system, psychiatric disorders, seizures, coma and death can occur.
The East African strain, named for the region that it is typically found, is the least common of the two with only a few hundred people becoming infected each year. This strain moves particularly fast, though, as patients see symptoms within 1-3 weeks and, if left untreated, death can occur within a few months. This strain is also a bit harder to control, as it is a zoological disease—several animals are able to host the parasitic strain.
The West African strain is the most common with 7,000-10,000 new cases reported each year. This strain can be hard to detect because symptoms can take up to a few months to surface and death can occur after the patient has been infected for several years. This strain, even with its prevalence, can be easier to contain, as humans are the primary hosts of infection. Effective treatment of infected humans will help stop the spread of the disease.
There are medications to help people combat the disease, but different medications are used depending on the stage of infection. Detection can be difficult and the medicine can be expensive, which makes treatment less accessible to those infected, as they reside primarily in rural areas. Spinal taps must be administered to ensure that the disease has not breached the central nervous system, which would cause the treatment plan to change. Even after a patient is considered cured, he or she must undergo routine screening, including a spinal tap, for up to two years. Even with precautions in place, relapse remains possible.
Even with few infected tsetse flies and a relatively small number of cases, the disease saw a resurgence of new cases after several years of latent activity. Nevertheless, the number of new cases are once again reducing every year; reports to the World Health Organization (WHO) have gone from 300,000 in 1995, down to just over 17,000 in 2004, below 10,000 in 2009 and only 7,139 in 2010.
Unfortunately, there is no vaccine available for HAT and recovery from a case does not result in immunity, yet progress is being made.
The WHO has taken great measures to aid African countries that are considered endemic: “technical assistance, access to diagnosis, training [and] access to treatment.” When these areas are focused on, things improve. Access to treatment has been a priority for the WHO because the medicine used for the second stage of the West African strain is an arsenic derivative. New treatments are being worked on to reduce the need for medicines that are accompanied by detrimental side effects.
Not every tsetse fly carries the disease, but the higher number of bites a person gets increases a person’s chance of becoming infected. The Centers for Disease Control (CDC) tells U.S. travelers to wear protective clothing when traveling in rural African areas with lots of brush, wear neutral colors that do not attract the flies, inspect vehicles for flies, avoid bushes, and use insect repellent. Repellent does not guaranteed protection against the tsetse fly, but it will help.
This disease’s resurged because it was ignored for a time. With the CDC’s suggestions and the WHO’s work in the field, the disease could become virtually non-existent in a short time if the decline seen in recent years continues. The medication used will help people gain their lives back and once again become productive members in their society. With all the good work being done to get rid of HAT, this disease could become a thing of the past in rural sub-Saharan communities.
– Megan Ivy
Sources: CDC, WHO, PLOS
Photo: the journal.ie
