Controlling Diphtheria Outbreak in Rohingya Refugee Camps
Since August 2017, the Rohingya refugee crisis has become an increasingly dire humanitarian issue. Nearly 700,000 Rohingya Muslims have fled Myanmar due to incidents of ethnic cleansing, and immigrated to the neighboring country Bangladesh.
Refugee Population in Bangladesh
As of mid-April, 781,000 refugees lived in nine different refugee camps and settlements, and an additional 117,000 in host communities away from the camps. This extreme population influx has made it hard for the Bangladeshi health system to properly pay for and accommodate for new public health risks associated with large refugee populations – including infectious diseases.
In response, large-scale vaccination programs have been introduced to decrease the risk of infectious disease endemics. By January 2018, over 300,000 children under the age of 15 had received a five-in-one vaccination that accounts for a variety of diseases including tetanus, whooping cough and diphtheria; however, that vaccine was not enough to protect said refugee population from infectious disease outbreaks.
Diphtheria in Refugee Camps
Despite vaccinations, diphtheria continued to remain a problem due to a lack of access to a vaccine booster -– immunity to the disease decreases every five years after the initial vaccination. In fact, a diphtheria outbreak was declared in November 2017.
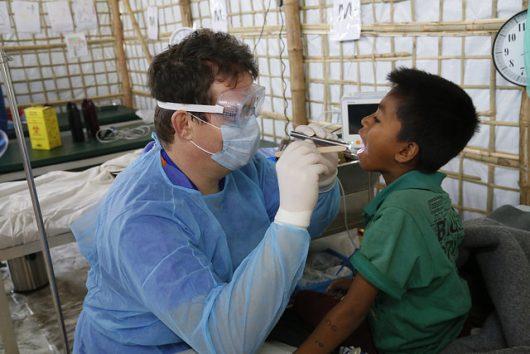
Diphtheria is a bacterial infection that causes thick covering along the back of the throat and leads to difficulty breathing, paralysis, heart failure and death. The bacteria produces a toxin that causes sore throats, weakness, fever, respiratory issues and swollen neck glands.
Rapid Outbreak
The first reported case was found in a Balukhali camp; however, at its height, the outbreak affected a number of refugee camps around 5000 acres of forested, undeveloped land –- over 150 suspected cases were reported daily.
Since its peak, the outbreak has now decreased to approximately 20 cases a day. The decrease is attributed to the establishment of effective treatment facilities, as well as contact tracing — a critical tool that enables healthcare officials to survey the spread of the disease, specifically, the employment of the World Health Organization’s (WHO) Early Warning, Alert and Response System (EWARS).
Early Warning, Alert and Response System
EWARS is meant to “improve disease outbreak detection in emergency settings” by utilizing modern technology to improve the efficiency and effectiveness of diagnosis and treatment in remote areas such as refugee camps.
Zarina Wong, a summer lab assistant at UCSF in the Cardiovascular Research Institute attests to the impact of digital networking, as it bridges the gap between old and new data. “This creates a lot of new opportunities for clinical research,” said Wong. “It can further inform doctors on how the disease may be spreading.”
The program collects disease alerts from over 150 primary health facilities across Rohingya refugee camps, as well as from the general public. Data is immediately uploaded when a utilized device is connected to the Internet.
The alerts are then reviewed, verified for accuracy and assessed for diagnosis. The diseases reported through this program include acute diarrhea, measles, mumps and diphtheria.
EWARS in a Box
WHO distributes EWARS in kits, known as “EWARS in a box,” that contain all of the equipment necessary to establish surveillance activity. The box contains 60 cell phones, “laptops and a local server to collect, report and manage disease data.” The kit also includes a solar generator in order to ensure that the phones and laptops provided function regardless of direct access to 24-hour electricity.
While the kits are pricey, they can support surveillance in up to 50 clinics (fixed or otherwise), serving roughly 500,000 people. The program has also been successfully implemented in Fiji, South Sudan and the Democratic Republic of Congo.
How Does Diptheria Spread?
Diphtheria is typically spread via respiratory droplets from coughing and sneezing. People can also get sick from contact with skin lesions or clothing of someone with diphtheria (a rare phenomenon).
According to the Center for Disease Control and Prevention, 10 percent of diphtheria patients die even after receiving treatment; nearly 50 percent die without treatment. The disease was one of the most common causes of death among children prior to the development of the diphtheria vaccine.
International Support
In addition to EWARS, the international humanitarian community released a joint response plan in March that called for $113 million to go towards Bangladesh’s health sector; however, less than 12 percent of the plan has been successfully funded. A combination of effective surveillance and funding must be maintained in order to provide for Rohingya refugees and their host communities.
Programs such as EWARS prove that community involvement and outreach make a huge impact on the containment of infectious disease such as diphtheria, one that is only enhanced by the technology guiding it.
– Katherine Anastas
Photo: Flickr
